Connecting with tiny patients:
Implementing developmental care
Facts about
preterm birth
Every year, an estimated 15 million babies worldwide — or more than 1 in 10 — are born preterm.¹ And every 30 seconds a baby dies of preterm birth.² In fact, preterm birth complications are the leading cause of death among children under 5 years of age, responsible for nearly 1 million deaths in 2013.¹ It is because of these startling statistics that Philips works to raise awareness on the importance of Developmental Care. Preterm infants have special needs, and carefully addressing those needs is key to their survival. They may need help breathing or maintaining body heat. Feeding can be challenging, and jaundice, low blood sugar, and anemia are all possible. They may also have difficulty dealing with stimuli, so the NICU environment is particularly important.



Developmental care in the NICU
This personalized approach includes educational programs for both mother and family. It also serves as a foundation for our Global Wee Care quality improvement program - a holistic methodology for managing stress and minimizing risk, which aims to provide a calming and soothing atmosphere that involves the whole family.
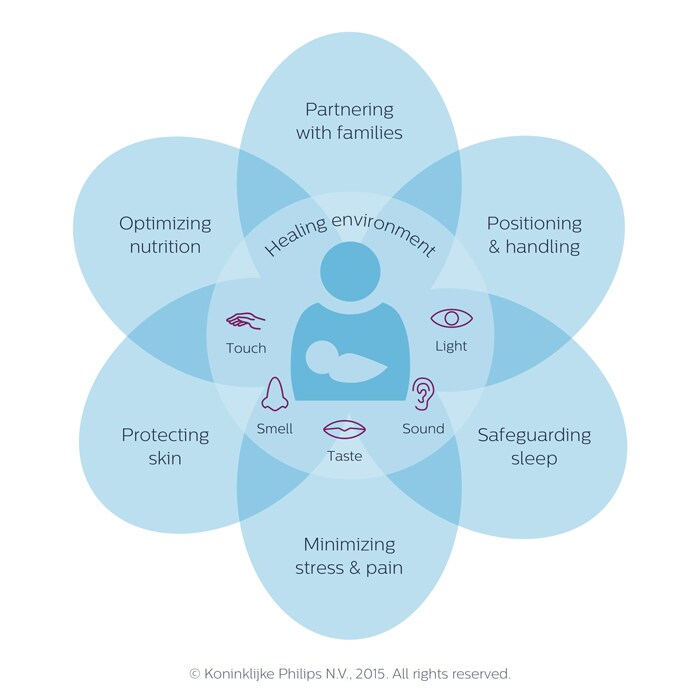
In addition to meeting the physical needs of infants in the NICU, it is also critical to meet their physiological and developmental needs. Our Integrative Developmental Care Model combines evidence-based best practices with core measures, and is one tool you can use to guide efforts to facilitate the physiological and developmental needs of each newborn.
Now our ward can be completely full and it is still very quiet and peaceful."
Dr. Carola Duijsters, Neonatologist, Maxima Medical Center, Veldhoven/Eindhoven, the Netherlands
Developmental Care in action
Developmental Care: A mother’s experience
Just as preterm infants must adjust to a world for which they are not yet developmentally prepared, so must their families adjust to an unexpected, and often highly clinical, experience. Teddy Blomstrom was born at almost 26 weeks. In the months that followed, as his mother Nanine learned about caring for her son, she also learned about Developmental Care in the NICU. Read more about Nanine’s personal perspective as a mother of a preterm infant.
Developmental Care webinars

Implementing Developmental Care
How does the NICU environment influence patients and parents? Hear current perspectives on implementing Developmental Care from Thomas Kühn, Neonatologist/Consultant at the Vivantes Perinatal Center in Berlin and CEO of Neotrainer.

Loma Linda University Children’s Hospital enhances its NICU environment and caregiving practices
Learn from Dr. Raylene Phillips of Loma Linda how they created a new NICU environment (physical, people, and processes) through nurse training and organizational transformation to improve delivery of care and patient satisfaction.
Related topics

Jaundice affects approximately 80% of preterm newborns, and 60% of all newborns.3
The high percentage of newborns who develop jaundice combined with the move towards shorter stays in the maternity ward requires increasingly innovative ways to diagnose and manage this common condition to avoid readmission.

Up to 60% of women who breastfeed stop earlier than they want to4.
The World Health Organization recommends exclusive breastfeeding up to 6 months of age5. But this very natural act does not come easily to every new mother. So it’s important that parents feel comfortable turning to you for expert advice.
